
Neither eye condition usually causes pain. Keratoconus causes astigmatism reducing visual acuity. Both may have astigmatism (eyesight problem of blurriness) present with keratoconus patients also sometimes experiencing myopia. With both diseases, eyesight deterioration progresses. Symptoms of Keratoconus and Pellucid Marginal Degeneration The first signs are often a minor blurring of their vision. Patients with keratoconus are often diagnosed sooner as vision starts to deteriorate earlier. Keratoconus will start to plateau after around age 40 but PMD will continue to progress. PMD symptoms will typically start to show after age 30. Symptoms of Keratoconus are often diagnosed in the teenage years. Many patients will have had a history of allergies, hayfever, asthma, or eczema, possibly due to excessive rubbing of the eyes. Some studies have found that PMD might be more apparent in women. Keratoconus is more likely to occur in men. About 3% of cases with corneal ectasia resulted in a PMD diagnosis with the other 97% having keratoconus. Keratoconus is quite a rare disorder and PMD is an even more rare eye disorder. There is often no hereditary link, but if you have a first-degree relative with keratoconus, you are at higher risk than the general population of developing this eye disease. It is a bit more complicated with Keratoconus. There is no known hereditary link for those with PMD. If the cone shape is away from the cornea, a patient with keratoconus can often be confused to have PMD. In PMD, cornea thinning extends 1–2 mm away from the inferior limbus while in keratoconus, the thinning usually occurs in the paracentral region. The cornea of a patient with keratoconus is cone-shaped rather than the dome shape of a healthy eye. It is sometimes referred to as a “beer belly” configuration when you view it from the side. 
This shows as the thinning of the corneal band with the cornea protruding above the thinning. PMD shows severe inferior crescent-shaped thinning of the cornea. Treating and managing these eye disorders is different so it is important to have a keratoconus or PMD specialist working with you to get the proper diagnosis. There is some discussion of whether PMD is a form of keratoconus or its own eye disease entirely. It is possible for a person to have both eye conditions but this is quite rare. While they may have similar topographic features, they have slightly different cornea abnormalities. Refract Corneal Surg 1989 5:414–7.Keratoconus and Pellucid Marginal Degeneration (PMD) are both considered to be cornea ectatic disorders or corneal thinning disorders. 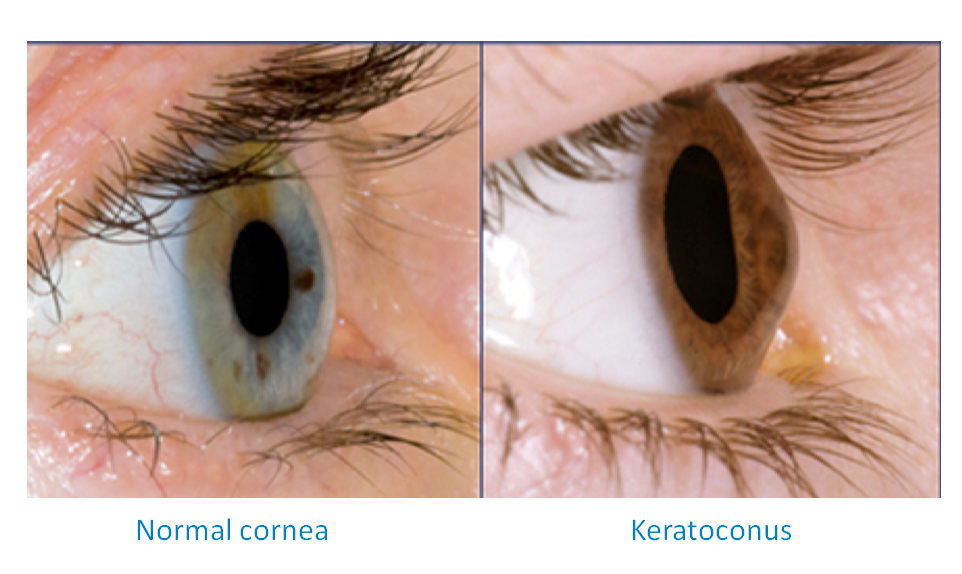
Corneal topography using rasterstereography. J Refract Corneal Surg 1994 10:103–11.Īrffa RC, Warnicki JW, Rehkopf PG. Characterization of the inherent error in a spherically-biased corneal topography system in mapping a radially aspheric surface. Corneal ectasia in vernal keratoconjunctivitis. Eur J Implant Ref Surg 1995 7:173–83.Ĭameron JA, Al-Rajhi AA, Badr IA. Terrien's marginal degeneration: corneal topography. Corneal topography of pellucid marginal degeneration. Maguire LJ, Klyce SD, McDonald MB, Kaufman HE. New York: Churchill Livingstone, 1988:498–9. In: Kaufman HE, Barron BA, McDonald MB, Walt-man SR, editors. The results of penetrating keratoplasty for pellucid marginal corneal degeneration. Epikeratoplasty for pellucid marginal corneal degeneration. Am J Ophthalmol 1983 96:253.įronterre A, Portesani GP. Crescentic lamellar keratoplasty for pellucid marginal degeneration. However, although the finding of PMCD and keratoconus in fellow eyes has been reported, to the best of our knowledge progression from PMCD to keratoglobus has not previously been shown. Keratoconus, PMCD and keratoglobus are considered to be associated as part of the spectrum of non-inflammatory corneal thinning disorders. Corneal topography suggested that in the second patient, PMCD may have preceded the development of keratoglobus. The other eye showed both clinically and topographically the features of PMCD. The second case had an uncommon presentation of hydrops in a clinically keratoglobic eye which showed a marked steepening of the inferior corneal periphery on corneal topography. The first case is a clinically typical bilateral PMCD with a characteristic pattern of irregular against-the-rule astigmatism on corneal topography. Although histopathologically it is considered a variant of keratoconus, it differs in that the marked corneal steepening occurs more inferiorly, above a narrow band of corneal stromal thinning concentric to the inferior limbus. Pellucid marginal corneal degeneration (PMCD) is an uncommon cause of inferior peripheral corneal ectasia, affecting patients between the ages of 20 and 40 years.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
